Your Medical Struggles Might Have a Psychological Component
Here’s what I’ve noticed about how my local clients and I often think about physical, mental, and emotional struggles: There’s primarily a medical fix and a spiritual safety net. Medical (or biological) first and spiritual as a kind of last resort.
If you’re feeling defensive or skeptical of where I’m headed already, let me validate myself a bit. I’m a nurse who worked in emergency departments for a few years before I decided I wanted to help people in a different way. So now I’m a therapist who practices in sort of a medical way, prioritizing treatments that have the most evidence from randomized controlled trials and integrating less structured, more difficult to study psychological approaches secondarily. I’m married to a pharmacist. We both have GI disorders for which we take medicine. I am not anti medical or anti medicine at all, and I am very much for seeing doctors to rule out diagnoses that could be addressed with medicine, surgery, supplementation, occupational therapy, physical therapy, speech therapy, etc. In fact, I encourage you to see a board qualified MD or DO at least once to be evaluated for whatever your medical concerns are before considering anything else I say in this blog.
BUT, sometimes the medical or biological approach is the only tool we have in the tool bag to address physical symptoms that might be worsened by our anxiety about our physical symptoms. Our anxiety may be increasing as we pursue more and more solutions that cause us to make more complicated, restrictive lifestyle alterations with the promise of eventually bringing relief if we get it just right.
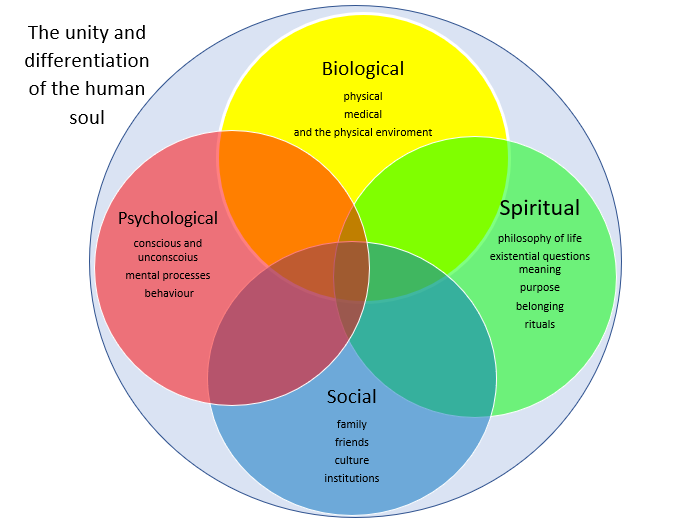
What we are missing is an understanding of ourselves as biological, spiritual, psychological, and social. Biopsychosocialspiritual is the one word term. That simply means that there are at least 4 parts or aspects of a person that have to be independently considered when you are trying to understand what they need to grow, improve, heal, and thrive. We all have our preferred emphasis that we understand and work with the best. Let me make a case for the importance of working on the psychological as it relates to health and the presence of physical symptoms. And I’ll give some thoughts about how this integrates with the spiritual as well.
Image Source: https://pastoralthinking.org/2023/01/20/relating-soul-to-spirit/
When The Biological Approach Alone Is Not Working
All stories are fictionalized to protect patient identities.
“I did a 16 week course on regulating my nervous system. It helped, but I still can’t do certain basic things I want to do because they make me so anxious. I feel so tense and exhausted all the time.”
“I’ve taken prescription anxiety medicines, seen a chiropractor, and worked with a functional medicine practitioner, but I still can’t sleep. I’m anxious all the time. I’m afraid my insomnia is going to cause dementia.”
“I try different diets where I eliminate certain allergens, dyes, and inflammatory foods, and they all work for a little while before my stomach starts to feel messed up again and I’m stressed about going places. I’m afraid I’m going to use the bathroom on myself in public, and I’m afraid I have some type of stomach or colon cancer.”
These are examples of people who have taken primary a biological (physical, medical, environmental) approach to their struggles with a malady that is presenting itself physically, such as anxiety, insomnia, and GI distress. But they aren’t getting the results they wanted, which is complete physical symptom relief and consequent removal of their anxiety and preoccupation with the symptoms.
They don’t really have a paradigm for how psychology could help them, or maybe they’ve already tried counseling and it hasn’t helped them.
I want to present some very basic ideas as to why the biological approach alone, when pursued too long and too intensely, may actually be making things worse rather than better and why certain counseling approaches sometimes don’t help if you find yourself in this situation.
How Intensely Pursuing a Fix Can Make Symptoms and Anxiety Worse
First, if you are not particularly anxious or preoccupied with your physical symptoms or the potential terrible results of your physical symptoms, this blog probably does not apply to you.
But if you are particularly stressed about your lack of sleep, IBS symptoms, panic attacks, subtle pains, or lightheadedness, and you regularly worry about what it means, how it might shorten your life, how it might cause dementia, or how you might embarrass yourself in public, please consider this. Your constant pursuit of a biological fix could actually be increasing your focus on your symptoms, stressing you out more, making your life smaller, and making your symptoms worse. If you’ve already had a doctor or two confirm, to the best of their ability, that it is nothing serious, then you should strongly consider the rest of this.
How Thinking and Behaviors Can Amplify Symptoms
We are going to use IBS and GI distress as our test case here, but you can creatively plug in whatever it is you are struggling with.
You’ve been tested for celiac disease, but you don’t have it. Sometimes you eat a bunch of pizza and you’re perfectly fine. Sometimes you eat it and it causes your guts to bubble and you notice your trip to the bathroom the next morning was slightly affected. So you cut out gluten for two weeks, and your morning trips to the bathroom straighten out, except for two days where they weren’t so great. So you cut out dairy as well for a week. It kind of helps except for Thursday when you got kind of anxious about having a bunch of gas at work from all of the fiber you’ve been eating and wondered if you should ask to work from home that day. Then you research the low FODMAP diet, but you aren’t desperate enough to try to pull that off. You’re on a treadmill of tinkering and researching that is producing mixed results. You’ve tried medicines to relax your gut, but you didn’t like the side effects.
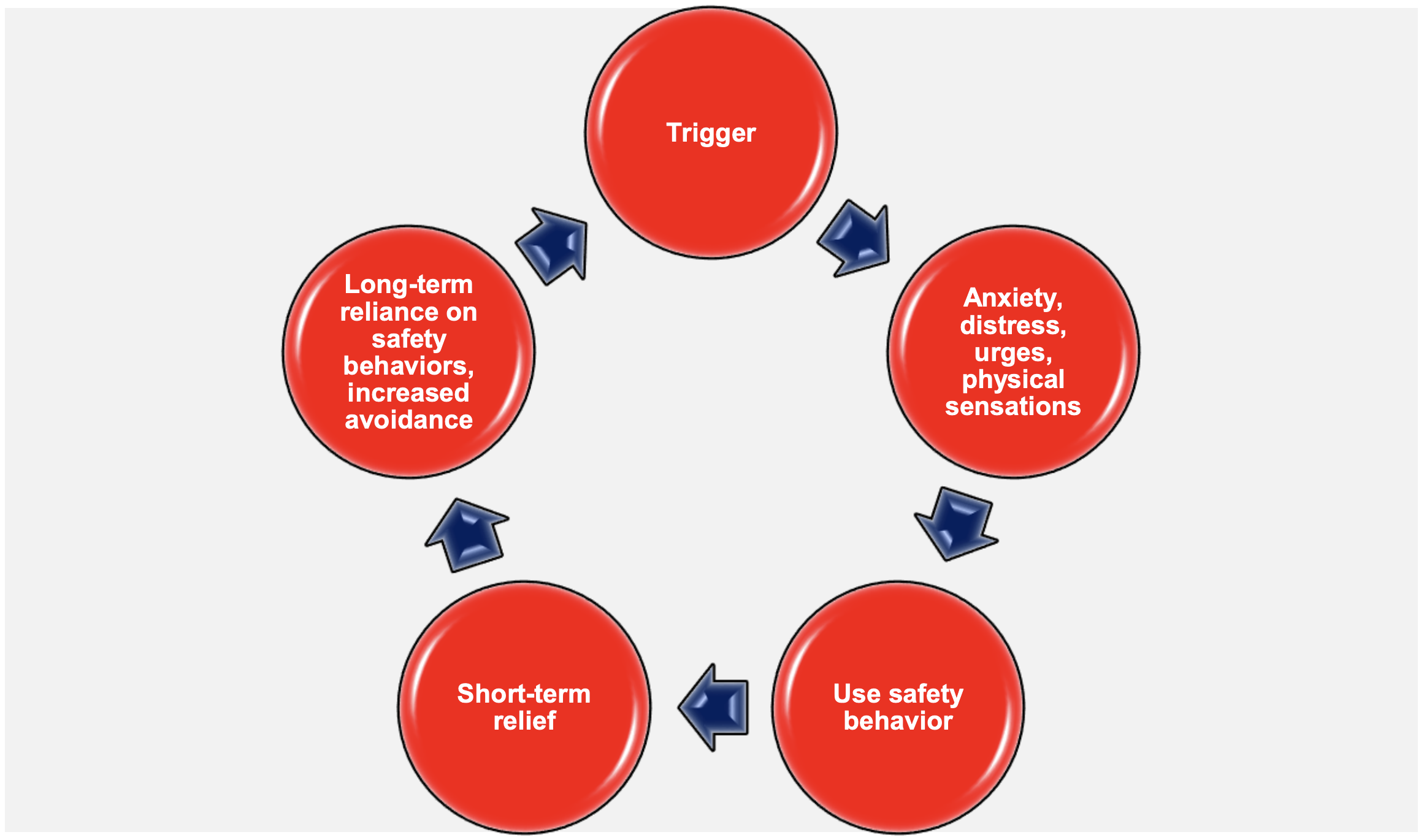
Many of these things you are trying could potentially be “safety behaviors” that are keeping you focused on your symptoms. There is a lot we could say about this concept, but let’s keep it very simple: The more you do about something, the more your mind focuses on that thing, monitors it, and worries about it.
Image Credit: Dr. Caitlin M. Pinciotti, Ph.D. - Baylor College of Medicine
Trigger: Guts are bubbling. Bloated.
Anxiety: “I’m going to be so embarrassed if I have to get up and go to the bathroom.”
Safety Behavior: Eat way less food than I actually want at dinner.
Short Term Relief: Avoided bathroom trip, and I believe that positive result came from eating just two bites of my dinner.
Long Term Issue: More diet and amount restrictions despite the fact that I have only once or have never had an embarrassing GI incident. More focus on and monitoring every sensation in my gut.
That’s the behavior focused angle.
Briefly, let’s look at how thinking and catastrophizing contributes to this cycle.
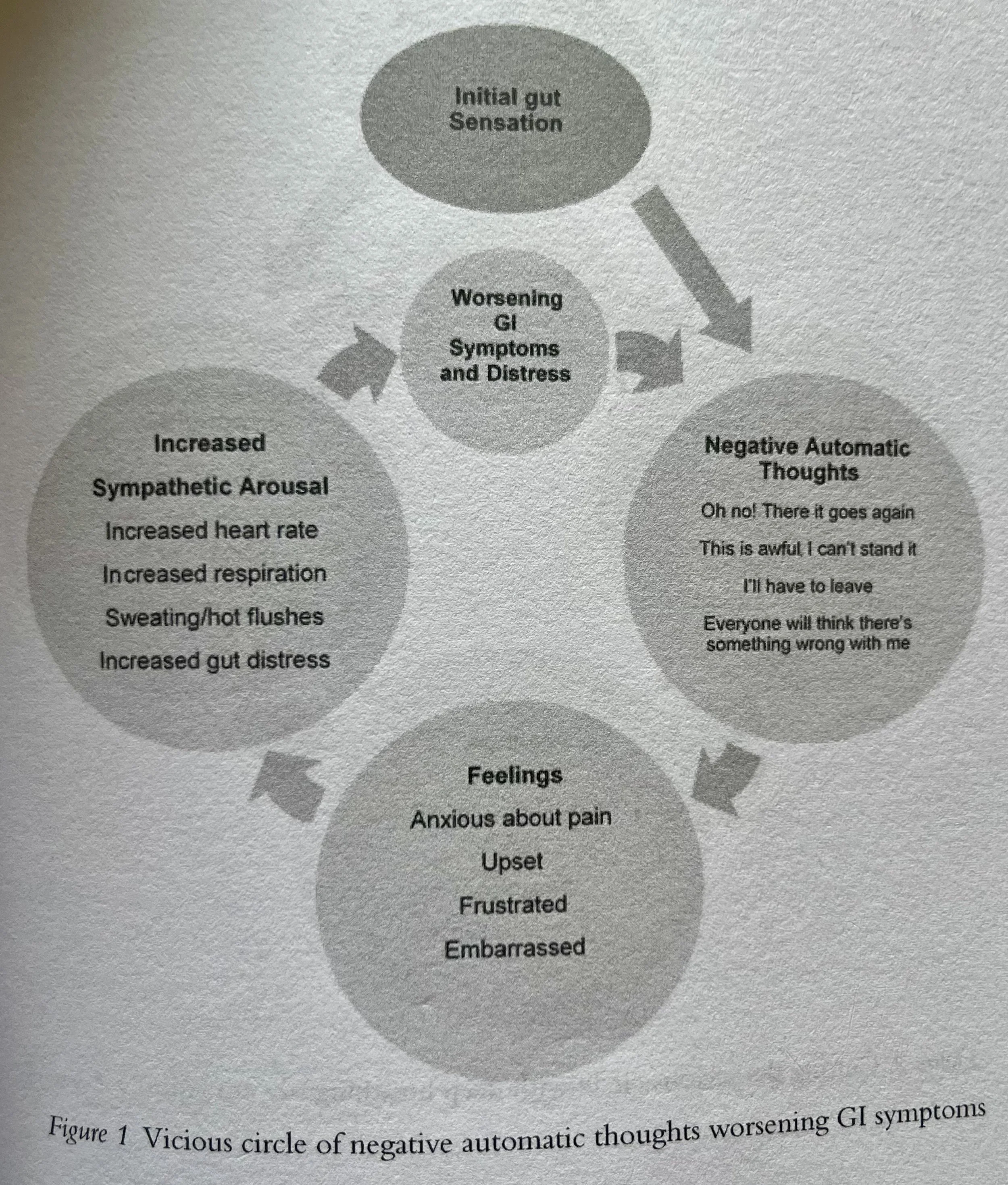
Image Credit: Hunt, M. G. (2022). Reclaim Your Life from IBS: A Scientifically Proven CBT-Based Self-Help Guide. Routledge.
Amazon Link: https://www.amazon.com/Reclaim-Your-Life-IBS-Scientifically-ebook/dp/B0B11LGB23?ref_=ast_author_mpb
This diagram focuses more on the role of how catastrophic, negative, or unrealistic thinking contributes to your distress, increases your anxiety, and causes a feedback loop where that generated anxiety worsens your GI symptoms.
In short, we must address both the thinking (cognitions) and actions (behaviors) that are amplifying your fear (emotion) and focus on whatever physical struggle you are having. This is the nuts and bolts of how cognitive behavioral therapy (CBT) works on the psychological component of what you are struggling with.
Thinking more realistically about the severity and meaning of your symptoms and doing LESS in response to your symptoms rather than MORE could be what you need to help the symptoms not be constantly front of mind and dictating your life. What often happens is that less focus on the symptoms via cognitive and behavioral restructuring causes your anxiety about them to decrease, which causes the increased symptoms that are caused by your anxiety and hypervigilance to decrease as well. Your threat detection system chills out, and often your symptoms chill out as well.
What Counseling Sometimes Misses
CBT is not the only psychological approach that can help if you relate to the idea that anxiety and preoccupation is making your physical symptoms worse, but it does have a large body of evidence behind it. I’m open to other approaches being helpful, and I sometimes refer clients out for other interventions if what I can do does not work for the client.
All of that said, what often happens that does not help these clients make progress is one of two things:
The only thing that is talked about is “why,” but not how to fix it. Maybe the therapist and client do some important exploration as to why they are so anxious, perfectionistic, concerned with health, or whatever it is going on. They relate it back to family dynamics, trauma, what was modeled to them, and desire for control. This is good and necessary, but insight should fuel and motivate a concrete plan of action to change how the person relates to their symptoms, not replace it.
Coping skills become the new safety behavior. When clients are distressed enough to come into therapy for this kind of problem, we feel for them. We should. They are miserable. That empathy and the presence of real symptoms sometimes keeps the therapist from gently pointing out that the client might be catastrophizing and pouring a little too much energy into trying to find biological solutions. So we settle for coping skills and never move on to getting them to challenge their thinking and minimize their attempts to eradicate the problem.
Sometimes you have to find a therapist who will push you gently and empathetically with a combination of grace and truth or else you won’t progress. Maybe more like a kind and persistent coach.
*Exposure and Response Prevention (ERP) is a special kind of CBT specifically for OCD. The principles here are still relevant for OCD, but OCD requires even more intense and strategic behavior change and cognitive restructuring. I describe that more here.
How Does This Relate to the Spiritual?
Jesus tells us not to worry about the future but instead to seek Him first and all of our needs will be taken care of because God loves us and knows what we need (Matthew 6:25-34). Mental ascent to that command is not going to get you very far. CBT is one way to begin enacting that process of not worrying so much, minimizing all of the extra effort you are putting in, and engaging in life with God instead of being completely engaged with your symptoms and fears. Doing less gives you the opportunity to learn the lessons I outlined here:
We have far less control of outcomes than we think we do
We underestimate God‘s ability and willingness to provide for us
We struggle to recall all the ways that God routinely and sometimes miraculously provides for us
We struggle to accept God’s grace for our sinful thoughts and motivations and worry about that instead of praying trustingly for God to change our hearts and minds.
We learn these things in a deeper way when we put ourselves in a position to experience them repeatedly, not just read them. Learning to trust God with our symptoms and practicing doing so helps us reduce our anxiety about them.
Start by Trying This
If you have read this far, then you probably relate to the idea that your anxiety about your symptoms is increasing your symptoms.
Start by simply identifying what you are preoccupied about. What have you already seen the doctor about and gotten reassurance, done a ton of internet research about, or can’t quit thinking about? For the next three days, I want you to really tune in and make some notes about how often you think about it and how much it distracts you from your regular life. Maybe make some notes about what your fear is related to it. Are you afraid that this is going to cause you to die an early death? Are you afraid that this will mess up your life satisfaction forever? Are you afraid that this is going to cause you to be embarrassed in public? Write those down as well. And ask yourself what solid evidence you have for those claims. Is it hearsay on social media and panic headlines from companies that are trying to get you to fall for their clickbait? Or is it the consensus of well informed experts and a lot of people with good common sense?
Finally, write down the minimum recommendations for helping the problem that you have. Choose just three or four. What I mean is this…If you relate to the content in this article, then you probably have extremely elaborate routines for addressing your symptoms. You might not even realize it, but you are probably doing or avoiding dozens of things a day. After your three day journaling process of building awareness, boil that down to just three interventions that have given you the most benefit or that medical experts agree are essential.
To stick with our IBS example, maybe dairy really does not work for you. So cut out dairy, only have one cup of coffee a day, and don’t eat past 8 PM. Other than that, don’t do anything else to accommodate your GI problems, especially don’t avoid situations and activities you enjoy. Commit to this for a month, and see what happens. This is a less is more approach. You may find that your symptoms improve drastically as your interventions and avoidance behaviors decrease. Even if that is not the result, thinking more clearly and realistically about what is going on with you and decreasing unnecessary interventions is going to expand your time and energy to engage who and what you love. That is the most important outcome of anything you do to improve your health.
About Us
Tyler Slay, LPC, is the founder of Anxiety & OCD Specialists of Mississippi, the first counseling clinic in the state dedicated exclusively to treating anxiety, OCD, and related disorders. As a specialist trained through the Behavior Therapy Training Institute (BTTI) of the International OCD Foundation (IOCDF), Tyler provides evidence-based care for adults, teens, and children. He and his team specialize in treating OCD, Anxiety, Panic Disorder, Tics/Tourette’s, and PTSD, integrating Christian counseling for those who desire a faith-aligned approach.
Contact & Location:
Clinic: Anxiety & OCD Specialists of Mississippi
Address: 100 Highpointe Dr., Suite D, Brandon, MS 39042
Services: In-person sessions in Brandon, MS and statewide via Telehealth
Credentials:View Tyler Slay’s Verified IOCDF Provider Profile